Lumbar Spondylolisthesis Pain - Fact Sheet
What is Lumbar Spondylolisthesis ?
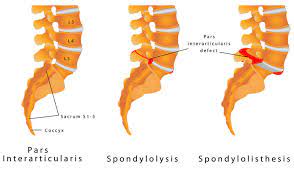
A “spondy” is a colloquial term for one vertebra that has slipped forwards on top of another. This can also be termed anterolithesis. This is due to one of three pathologies: Spondylosis, Spondylolysis, or Spondylolisthesis.
Spondylosis is the most common form of spondy in the lumbar spine. This is where osteoarthritic changes of the vertebrae themselves contribute to the movement of one vertebrae on another.
Spondylolysis refers to a stress fracture or defect of the pars interarticularis – a small bony structure of the lumbar vertebrae. This may or may not lead to a Spondylolisthesis, which refers to a vertebra defect that can allow a vertebra to slide over another when aggravated by certain activities. This is most common at the L5/S1 level. Spondylolisthesis is common in the younger athlete as a result of stress fracture.
What causes Lumbar Spondylolisthesis ?
- Repetitive, uncontrolled loading of the spinal structures in combination with backward bending and rotation of the spine
- Excessive training (loading) with a lack of control/stability of the spine
- Poor muscle strength and flexibility
- In cases of spondylosis, normal ageing/degenerative changes of the spine
.
Signs and Symptoms of Lumbar Spondylolisthesis?
- Back pain just to one side of the spine or on both sides
- Pain following provocative activity/sport, which lessens with rest
- Pain increases and limited range of movement when leaning backwards or bending to the side
- Pain when pressing on the area
- If there is compression of the spinal cord or a nerve, this may cause pain, numbness, pins and needles, changes in sensation in the buttocks and legs.

Treatment and Management Lumbar Spondylolisthesis?
Initially: avoiding aggravating activities, such as backwards bending/arching
Rest or modified training: avoiding provocative movements in your chosen sport, and replacing these in the short term with activities that promote pain-free movement, reducing the amount of stress placed on the spine (water-based activities and cycling are better options than running and walking). Seek an opinion from an MD Health Physiotherapist or Exercise Physiologist if you are unsure about what is appropriate.
Lumbar flexion movements, exercise: Stretching the muscles surrounding the spine in a forwards movement, bringing knees to chest and rotation the hips side to side can provide some relief as this takes the pressure off the irritated areas.
Stability exercises: strengthening exercises of the deep and superficial abdominals, lumbar stabilisers and extensors, and the gluteal muscles can help improve the stability and control of the spinal segments. With symptomatic spondys, these exercises should be supervised for correct technique.

Prognosis/Recovery Lumbar Spondylolisthesis?
Depending on the severity of the spondy, healing time may vary. In some cases, complete healing may not occur, therefore, receiving adequate physical rehabilitation treatment is an essential part of recovery to ensure that there is enough muscle support post injury to avoid reoccurrence and compensatory issues to develop. Generally, bones should re-unite after six to 12 weeks. Surgical interventions are not usually required but in severe cases, they may be advised.

Red Flags for Prognosis/Recovery Lumbar Spondylolisthesis?
If any of these symptoms develop (either initially or down the track in your recovery) please seek medical advice immediately:
- Severe pain + pins and needles and/or numbness extending in the buttocks or legs
- Lack of bladder/bowel control and/or loss of sensation in the buttocks and pubic area
- Progressive weakness in the legs, pain with normal walking (claudication)
- Severe, continuous abdominal and low back pain
- Fever, chills, history of cancer, pain waking you up at night, sudden weight loss, recent severe trauma
no noticeable reduction in pain and inflammation after 72 hours of self-care



