When it comes to osteoarthritis (more commonly referred to as OA) it can be confusing with all the information out there of the best way to treat it – What works? What doesn’t? In this article we will seek to answer questions you may have about Osteoarthritis and what works and what doesn’t in relation to rehabilitation and treatment.
Osteoarthritis (OA) of the knee is a major cause of pain and locomotor disability worldwide. In January 2010, the OA Research Society International (OARSI) published an update to their evidence-based, consensus recommendations for the treatment of OA of the hip and knee.
Since the publication of the 2010 OARSI guidelines, the evidence base on knee OA treatment has evolved. This guidelines statement aims to incorporate evidence from these recent publications, in addition to the best-available previously published research, to assess where previous treatment recommendations should be modified or expanded to include new OA treatments. As clinical considerations and availability of evidence between knee OA and hip OA treatments differ, the present guidelines sought to focus specifically on treatment of primary OA of the knee.
OA Research Society International (OARSI) Guidelines
For the present guidelines, the aim was to determine the most applicable treatment recommendations by narrowing down the relevant comorbidities. Comorbidities are the presence of one or more additional conditions co-occurring with a primary condition, in this case OA, and examining for the presence of OA in joints other than the knee(s).
This statement updates the previous OARSI recommendations, incorporating literature published between January 2009 and March 2013. Its aim is to examine the safety and efficacy or effectiveness of new therapies for OA and re-examine existing therapies considering recent evidence. These recommendations are intended to be used in conjunction with individual client and practitioner’s values and judgments to optimise OA treatment for different individual needs.
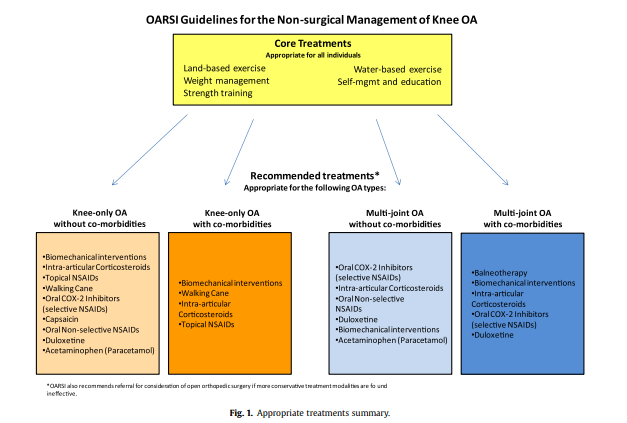
The following table displays considerable listed therapies (according to client needs);
In summary, What Works?
Strength training (Both weight-bearing and non-weight-bearing) –
Tailored strength training both individual and group (moderate effect on pain/function with strong evidence)
Weight Management (>5% loss of body weight) –
(Low—Moderate effect on pain/function with strong evidence)
NSAIDS and Opioids –
(Low – Moderate Effect on pain with strong evidence)
Joint Replacement –
(High effect on pain/function with strong evidence, but no placebo-controlled trials)
What Doesn’t Work?
Massage, Laser, ultrasound treatment –
(Poor effect on pain/function with good-moderate evidence, still confirming these results)
Surgical Arthroscope –
(Poor effect on pain/function with strong evidence to support)
Do you have any questions?
- Call us on (03) 9857 0644 or (07) 3505 1494 (Paddington)
- Email us at admin@mdhealth.com.au
- Check out our other blog posts here
Our clinical staff would be happy to have chat if you have any questions.