Plantar Fascia Pain - Fact Sheet
What is Plantar Fascia Pain?
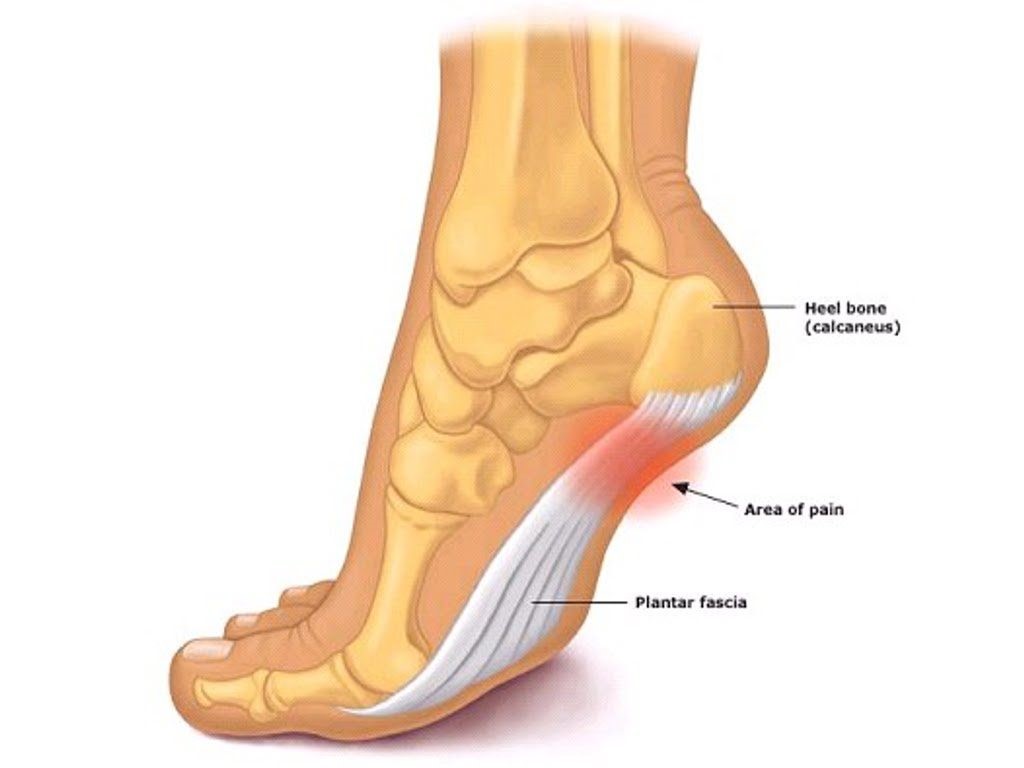
The Plantar Fascia is a tendon-like structure that runs from your heel along the sole of your foot. This structure provides stability to the medial arch of the foot, particularly with gait (walking), running and jumping. If the plantar fascia is subjected to loads that it cannot tolerate, irritation and breakdown of the fascia can occur, leading to pain +/- inflammation.
What causes it?
Spikes in load that the plantar fascia cannot tolerate (such as a sudden increase in training, walking long distances in inappropriate footwear, or increase in jumping/changing direction activities) can lead to irritation and breakdown of the plantar fascia tissue. this can be referred to as Plantar Fasciopathy (previously plantar fasciitis). However, acute strains of the plantar fascia can occur as well, where you may feel a small pop in the sole of the foot following by pain, bruising, and pain with walking. This would be more indicative of a plantar fascia strain. In both cases, the treatment remains similar.
Signs and Symptoms of Plantar Fascia Pain?
• Pain at the sole of the foot or on the heel (generally medial to the heel itself as pictured)
• Pain with the first few steps in the morning, which gets better as you get moving.
• Pain after long walks or running
• Pain with wearing footwear that is too flat or provides little support
Treatment of Plantar Fascia Pain?
Activity modification – Reducing or modifying any aggravating activities or exercises. As a general rule, pain shouldn’t be higher than 3-4 out of 10 either during or after any given activity or exercise. If this is higher, the load/intensity of this exercise needs to be reduced.
Isometric Exercises, or ISOs – In the initial stages of rehab, Isometrics (or ISOs) of the calf/foot muscles (specifically targeting the plantar fascia itself) can help gradually build-up load capacity again with low risk of re-injury or pain flare-ups. In fact, ISOs can also have an analgesic effect on the fascia tissue, reducing pain immediately after the exercise. An Exercise Physiologist or Physiotherapist can help guide you on the correct dosage and intensity of your ISO exercises.
Gradual return to full activity – As pain permits, slow re-introduction into full load-bearing range of movement exercises of the foot and ankle. Again, pain levels should not rise to higher than 3 or 4 out of 10 when these types of exercises get introduced. Once these are more tolerable, a gradual return to full activity can start to occur. If you are returning to sport, introduction of plyometric (jumping and landing) exercises is strongly recommended.
Other options – if exercise-based treatment and activity modification doesn’t work in the medium-term (6-12weeks), local injection of corticosteroid into the fascia can help reduce the pain. However, this doesn’t fix this issue, as the muscle/fascia is still quite weak. What this CAN do is provide a relatively pain-free window to strengthen these tissues again without flare ups of pain, so that this does not become a recurring issue.



